June 2012 Arizona Thoracic Society Notes
 Thursday, June 28, 2012 at 11:53AM
Thursday, June 28, 2012 at 11:53AM The June 2012 Arizona Thoracic Society meeting was held on 6/27/2012 at Scottsdale Shea beginning at 6:30 PM. There were 23 in attendance representing the pulmonary, critical care, sleep, pathology, infectious disease, radiology, and thoracic surgery communities.
Discussions were held regarding offering CME and partnering with other thoracic societies in the Southwest Journal of Pulmonary and Critical Care. This was endorsed by the membership. There was also discussion regarding what to discuss with Rep. David Schweikert on August 8.
Seven cases were presented:
- Thomas Colby, a pulmonary pathologist from the Mayo Clinic, presented a case of a 45 yo woman with a history of asthma and systemic lupus erythematosis who was found to have cysts on CT scanning. The CT scan was considered consistent with lymphangioleiomyomatosis (LAM). A lung biopsy showed only changes consistent with asthma in addition to the cysts. This case was published along with 4 similar cases by Rowan C, et al. Am J of Surg Pathol 2012;36:228–34.
-
Jonathan Ruzi, a pulmonologist and sleep medicine specialist in Scottsdale showed an unusual flow-volume loop in an asymptomatic patient (Figure 1 below).
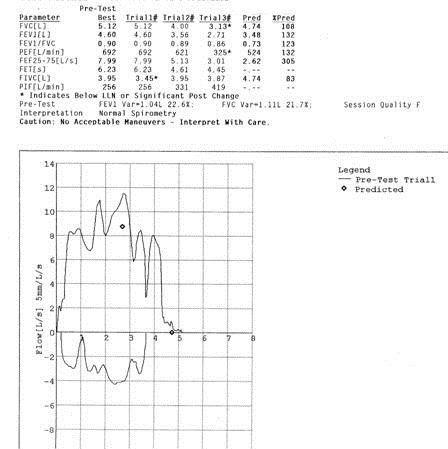 Figure 1. Flow-volume loop of patient presented in case 2. The cause of the obstruction was unknown but most thought this represented a type of upper airway obstruction from redundant tissue such as seen in obstructive sleep apnea or an enlarged tongue.
Figure 1. Flow-volume loop of patient presented in case 2. The cause of the obstruction was unknown but most thought this represented a type of upper airway obstruction from redundant tissue such as seen in obstructive sleep apnea or an enlarged tongue. - Henry Luedy, a pulmonary fellow, presented a case of an 82 yo with cough who was a former smoker with COPD who presented with a cough. The patient presented with a consolidative process in the lingula and underwent bronchoscopy which revealed bronchial inflammation and a trace of blood in the lingula. Biopsy revealed an adenocarcinoma. Unfortunately, the pathology was not presented due to Dr. Luedy being unable to obtain the slides or images from the VA due to a clerk citing HIPAA regulations as the reason. A discussion was led by Dr. Colby on how the pathology affects the classification of these tumors as bronchoalveolar or adenocarcinoma and how there is much overlap between the classification. It was noted that educational activities are excluded from HIPAA regulations as long as the data is de-identified and there are not identifiers on a pathology slide.
- Tonya Whiting, a pulmonary fellow, and Manny Mathew, a pulmonologist based at Good Samaritan, presented a case of a man who developed shortness of breath while camping in the White Mountains. CT scanning revealed dense consolidation especially of the left upper lobe. He was referred for bronchoscopy but both his symptoms and consolidation resolved within 24 hours. It was felt this was a case of high altitude pulmonary edema which was somewhat unusual because high altitude pulmonary edema is unusual below 12000 feet (the patient was camping at about 9000 feet).
- Tonya Whiting and Allen Thomas, a pulmonologist at the VA, presented a 61 year old man with a history of polysubstance abuse and multiple lung nodules. Bronchoscopy with bronchoalveolar lavage and transbronchial biopsy was negative. Open lung biopsy revealed brochiolcentric inflammation with acute lung injury. The patient was treated with corticosteroids and the nodules resolved in 2-3 weeks. The feeling was that this represented cryptogenic organizing pneumonia (COP) presenting with multiple nodules which is a rare presentation for COP.
- Andrew Goldstein, a thoracic surgeon, presented a case of a 50 year old asymptomatic, nonsmoker with a huge, > 10 cm, lung tumor. The lesion was round and smooth and did not invade the chest wall on CT scan. Dr. Goldstein pointed out that pain is sensitive in predicting chest wall invasion. The tumor was resected and proved to be a carcinoid tumor.
- Tim Kurberski, an infectious disease specialist from Maricopa Medical Center, presented a 39 year old with a history of systemic lupus erythematosis on corticosteroids who presented with shortness and breath thought to be secondary to pulmonary edema from a cardiomyopathy. The CT scan revealed diffuse ground glass opacities. The patient also had a rash near the buttocks which was thought to be possible shingles and the chest findings possible chickenpox pneumonia. The steroids were increased but the patient failed to improve. She underwent bronchoscopy with bronchoalveolar lavage which revealed larvae consistent with Strongyloidiasis.
There being no further cases, the meeting was adjourned at 8:30 with the next meeting being a special meeting on August 8 when Rep. David Schweikert is scheduled to attend.
Richard A. Robbins, M.D.
CCR Representative
Arizona Thoracic Society
Reference as: Robbins RA. June 2012 Arizona Thoracic Society notes. Southwest J Pulm Crit Care 2012;4:211-3. (Click here for a PDF version of the Notes)
