Pulmonary Hantavirus Syndrome: Case Report and Brief Review
 Monday, September 28, 2015 at 1:19PM
Monday, September 28, 2015 at 1:19PM Charles J. VanHook, MD
Britt Warner, PA
Angela Taylor, MD
Longmont United Hospital
Longmont, Colorado
A 31-year-old white man presented to the emergency department complaining of fever, headache, mild confusion, and muscle aches. Approximately three days earlier he had developed non-quantified fever and diffuse muscle aches and pains. He was employed as a feedlot worker. He had visited an urgent care center one day earlier and had been advised to increase his oral fluid intake and to use non-steroidal anti-inflammatory agents as needed. Upon arrival to the emergency department he was found to have a temperature of 103.6º Fahrenheit, blood pressure of 125/72 mm Hg, respiratory rate of 40 breaths per minute, and room-air oxygen saturation of 84% by pulse oximetry. Auscultation of the chest disclosed diffuse rales. Heart sounds were rapid and regular. Abdominal exam was benign. There was no skin rash. Central nervous exam demonstrated agitation and confusion, but was otherwise non-focal. Laboratory examination revealed a white blood count of 11.7 K/uL, hemoglobin of 21.5 g/DL, hematocrit of 66.8%, platelet count of 73 K/uL, partial thromboplastin time of 36 seconds, lactic acid of 2.4 mm/L, and procalcitonin of 43 ng/mL. Chest radiograph disclosed extensive bilateral infiltrates (Figure 1).
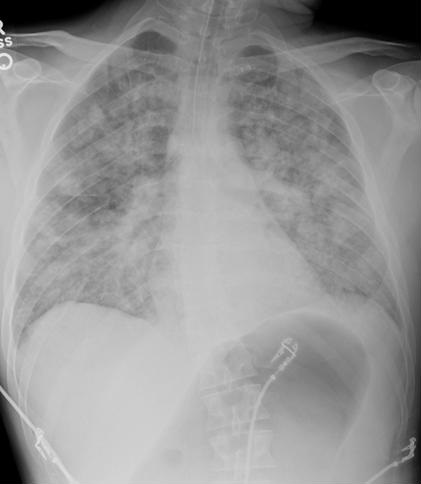
Figure 1. Chest x-ray showing bilateral infiltrates
The patient precipitously declined, with severe respiratory distress, and was emergently intubated. Despite aggressive measures, including mechanical ventilation with an FIO2 of 1.0 and PEEP of 18 cm H2O, vigorous intravenous intravenous fluid resuscitation with normal saline, and pressor support with intravenous norepinephrine and vasopressin, the patient developed refractory hypoxemia. This was followed by a bradycardic arrest and death 2 hours after presentation. Serology sent at the time of admission later returned as IgM positive for hantavirus, with subsequent testing positive for Sin Nombre IgM.
Hantaviruses are RNA viruses of the family Bunyaviridae that are transmitted to humans by contact with the saliva, urine, or feces of infected rodents, which serve as persistently infected hosts (1). Patients who work in proximity to rodents, such as animal trappers, farmers, and forestry workers are at highest risk for infection. In the Western Hemisphere, there are approximately 200 cases per year of Hantavirus Pulmonary Syndrome (HPS), which was first identified in the Four Corners area of the Southwestern United States in 1993 (2). In the United States, HPS is most commonly caused by the Sin Nombre subfamily of hantavirus. A two-week incubation period precedes a 3-6 day prodromal period during which fever and myalgia are prominent features. The cardiopulmonary phase of HPS follows, with the development of acute non-cardiogenic pulmonary edema and multi-organ dysfunction. Typical laboratory abnormalities are leukocytosis and thrombocytopenia. Elevations in hematocrit and partial thromboplastin time are strong predictors of mortality, which approaches 40%. Definitive diagnosis depends on the serologic identification of IgM antibody to hantavirus using ELISA technology. Immunochromatographic technology may allow for same day diagnosis (3). Treatment is supportive, and varies with the severity of disease. It may include volume resuscitation, ventilatory support, and renal replacement therapy. There is no established anti-viral therapy for Hantavirus infection, although ribavirin is often used in Asia. Corticosteroids have also been used sporadically with some success, but their use remains controversial (3).
Although Hantavirus remains a rare disease, prodromal symptoms in a patient with associated epidemiologic risk factors should heighten clinical suspicion.
References
- Lednicky JA. Hantavirus: A short review. Arch Pathol Lab Med. 2003;127:30-35. [PubMed]
- Duchin JS, Koster FT, Peters CJ, Simpson GL, Tempest B, Zaki S, Ksiazek TG, Rollin PE, Nichol S, Umland E, Moolenaar RL, Reef SE, Nolte KB, Gallaher MM, Butler JC, Breiman RF. Hantavirus pulmonary syndrome: a clinical description of 17 patients with a newly recognized disease. N England J Med 1994;330:949-55 [CrossRef] [PubMed]
- Bi Z, Formenty P, Roth C Hantavirus infection: A review and global update. J Infect Developing Countries. 2008;2(1):3-23. [CrossRef] [PubMed]
Cite as: VanHook CJ, Warner B, Taylor A. Pulmonary hantavirus syndrome: case report and brief review. Southwest J Pulm Crit Care. 2015;11(3):121-3. doi: http://dx.doi.org/10.13175/swjpcc122-15 PDF

Reader Comments