The end of the year has traditionally been a time to reflect on the top stories of the year. Here's our list of the top local medical stories.
1. VA scandal
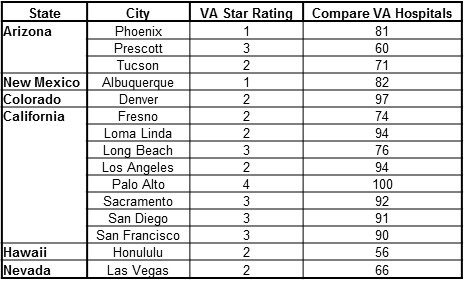
Phoenix was the epicenter of the VA scandal but Albuquerque and the Greeley, Colorado clinic also figured prominently in the falsification of patient wait lists. Investigations revealed that at least 70% of the VA hospitals falsified records leading to the resignation of VA secretary, Eric Shinseki, and his under secretary for health, Dr. Robert Petzel. Eventually the director of the Phoenix VA, Sharon Helman, was fired-not for the falsification of medical records but for taking inappropriate gifts. However, most of the directors of the VA hospitals that falsified data remain untouched, still receiving their bonuses. Similarly, the politicians, the inspector general and those in the VA central office whose job was to provide oversight remain unscathed. On the bright side, the scandal did result in a modest influx of monies which hopefully will be spent on patient care rather than administrative bonuses.
2. Ebola outbreak
This seems a bit odd for a local news story but the Ebola epidemic in Africa did impact locally. The outbreak was largely ignored by the American public until a patient and several healthcare workers became infected in the US. Politicians and healthcare administrators seized the opportunity to hype the hysteria and insist on training of healthcare workers. One Arizona Thoracic Society meeting was cancelled because a nursing service needed the room to do "Ebola training". As Peter Sagal said on "Wait, Wait, Don't Tell Me" there have been more Americans married to Larry King that infected with Ebola illustrating the hysteria and resultant overreaction. This year's true medical heroes are the thousands of physicians and nurses who worked on the frontlines of the Ebola crisis in Africa at tremendous personal risk and despite chaotic conditions, underequipped facilities, and overwhelmed local health systems. In contrast to the politicians and healthcare administrators, Anthony Fauci has consistently offered reasonable recommendations and insight based on science.
3. Banner Health, University of Arizona Health Network merger
In June, the Banner Health and University of Arizona Health Network (UAHN) began negotiations to merge with Banner absorbing UAHN's $146 million debt. Banner promised to spend at least $500 million toward capital projects in the next five years and pay $300 million to establish an academic endowment. The deal is to be completed about the end of January, 2015. Mergers between the private and public health sectors have been a mixed bag and this one warrants close watching.
4. Meaningful use
Many physicians suspected that the Centers for Medicare and Medicaid Services' (CMS) meaningful use was little more than a scheme to have physicians perform useless clerical tasks. When they were not done, payment would be denied. At the end of 2014 this appears to be true. There remains no data that the meaningful use is "using certified electronic health record (EHR) technology to: Improve quality, safety, efficiency, and reduce health disparities" as intended. About 257,000 physicians will receive a 1% reduction in reimbursement in 2015.
5. Reduction in CMS hospital payments
Despite the lack of data that CMS' value-based healthcare program is doing much to benefit patients and some data that performance of the measures has been associated with adverse outcomes, CMS continues to reduce hospital payments because of hospital-acquired conditions and high readmission rates. We initially reported on this in June, 2013. We are not advocating for hospital-acquired infections or readmissions, but are advocating for measures that improve patient outcomes. Despite a phone call assuring us that CMS would look into it, nothing has seemed to change. Furthermore, much of the data is self-reported by the hospitals. As the VA scandal illustrates, self-reported data is not always reliable especially when money is involved.
6. Congress again fails to pass SGR fix
Congress passed a budget but failed to fix the widely hated sustainable growth rate (SGR) formula for physician reimbursement under Medicare. Also missing was an extension of the current pay bump for primary care. SGR has been present since 1997 and the one of the few things the politicians seem to come together on is not paying physicians, especially primary care physicians, a decent living wage.
Richard A. Robbins, MD
Editor
Southwest Journal of Pulmonary and Critical Care
Reference as: Robbins RA. 2014's top southwest medical stories. Southwest J Pulm Crit Care. 2014;9(6):350-1. doi: http://dx.doi.org/10.13175/swjpcc167-14 PDF
 Thursday, December 15, 2016 at 8:00AM
Thursday, December 15, 2016 at 8:00AM