January 2020 Critical Care Case of the Month: A Code Post Lung Needle Biopsy
 Wednesday, January 1, 2020 at 8:00AM
Wednesday, January 1, 2020 at 8:00AM Sarika Savajiyani MD and Clement U. Singarajah MBBS
Phoenix VA Medical Center
Phoenix, AZ USA
A 67-year-old man with a history of stage IIA rectal adenocarcinoma post neoadjuvant chemoradiation presented with a near code event after elective CT guided biopsy of an enlarging left lower lobe lung nodule. The patient became bradycardic and profoundly hypotensive immediately after the CT guided biopsy with the following vital signs: Systolic BP < 90 mmHg, HR 40/min sinus bradycardia, SpO2 on 100% oxygen non rebreather was 90%. Telemetry and EKG showed ST elevation in the anterior leads. He complained of vague arm and leg weakness and tingling, but did not lose consciousness or suffer a cardiac arrest.
A CT scan was performed about 2-3 minutes after the patient deteriorated (Figure 1).
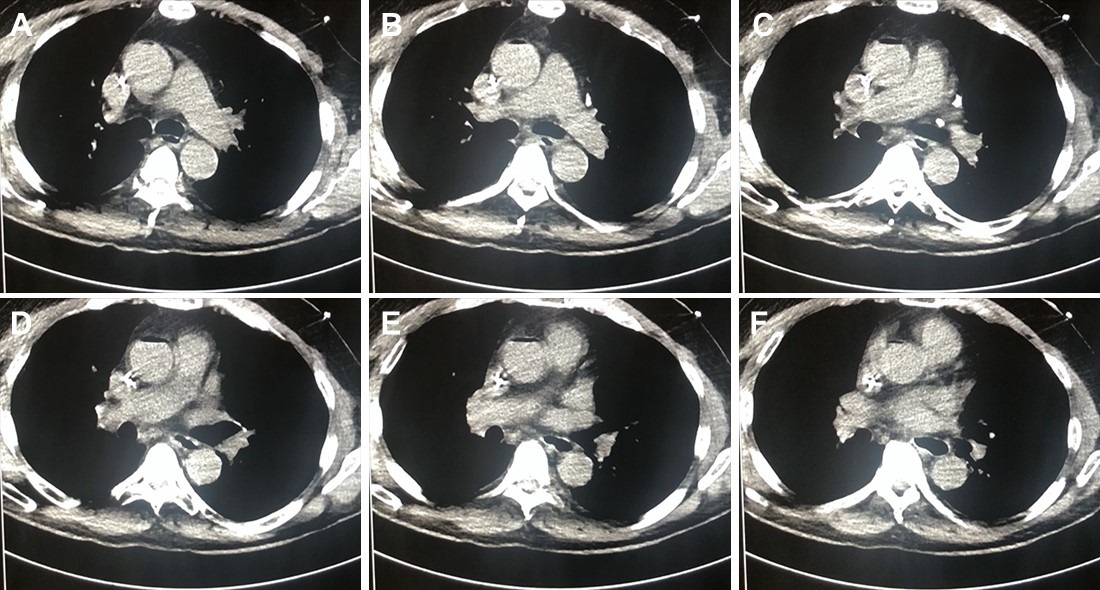
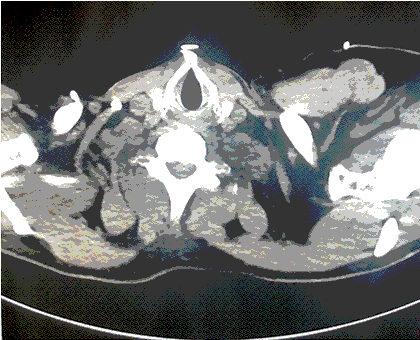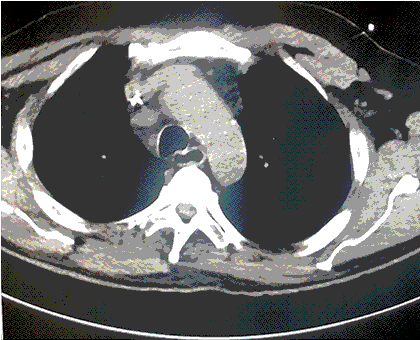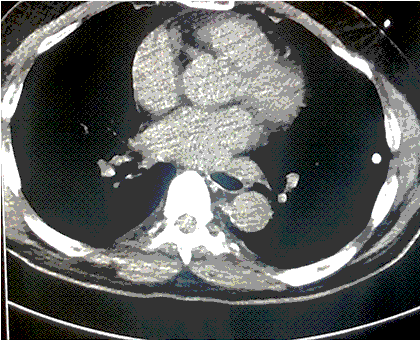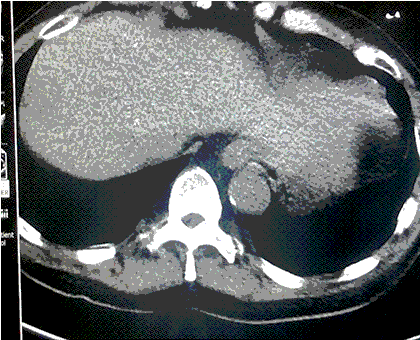
Figure 1. A-E: Representative images from CT scan in soft tissue windows. Lower: Video of CT scan in soft tissue windows.
What radiographic finding likely explains the patient’s clinical deterioration? (Click on the correct answer to be directed to the second of six pages)
Cite as: Savajiyani S, Singarajah CU. January 2020 critical care case of the month: a code post lung needle biopsy. Southwest J Pulm Crit Care. 2020;20(1):1-6. doi: https://doi.org/10.13175/swjpcc042-19 PDF

Reader Comments