April 2017 Critical Care Case of the Month
 Sunday, April 2, 2017 at 8:01AM
Sunday, April 2, 2017 at 8:01AM Robert A. Raschke, MD
Banner University Medical Center-Phoenix
Phoenix, AZ USA
History of Present Illness
A 20-year-old woman was transferred from another medical center for care. She was pregnant and initially presented with a one day history of crampy abdominal pain with nausea and vomiting after eating old, bad tasting chicken two days previously. She had pain of her right arm and a non-displaced humeral fracture was seen on x-ray. The etiology of the fracture was unclear. Her illness rapidly progressed to respiratory distress requiring intubation. The fetus had deceleration of heart tones leading to a cesarean section and delivery of a non-viable infant. Subsequently, she had rapid progression of shock and anuria.
Past Medical History
She had a previous history of a seizure disorder which was managed with levetiracetam, clonazepam, and folic acid. There was a previous intentional opiate overdose 2 years earlier. One month prior to admission she had visited her husband in Iraq. After returning to the US 3 weeks prior to admission, she developed a sore throat and was treated with penicillin. She smokes tobacco hookah and marijuana. There is a positive family history of gout.
Physical Examination
- Vital signs: heart rate 109, blood pressure 102/78 mm Hg while on norepinephrine, respiratory rate 22, temperature 36.5º C.
- General: She was sedated and intubated. She had a splint on her right arm.
- Lungs: clear anteriorly
- Heart: regular rhythm without murmur
- Abdomen: firm without palpable organomegaly or masses.
- Neurological examination: There was movement of all extremities. Muscle tone was normal. Deep tendon reflexes were normal. Plantar reflexes were down going.
- Skin: diffuse erythematous macular popular rash on the trunk and back (Figure 1).
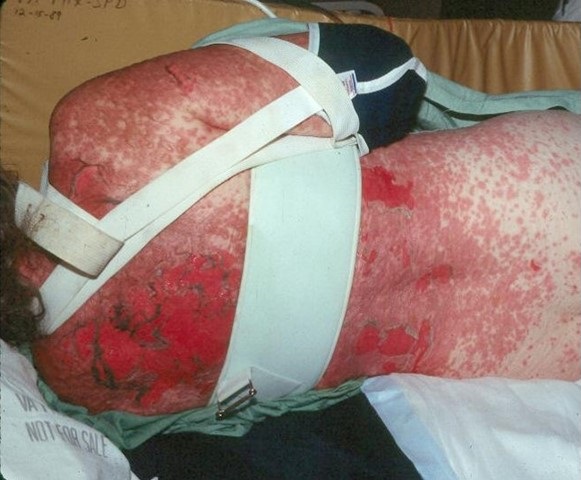
Figure 1. Photograph of patient’s back showing rash.
Initial Laboratory Evaluation
- CBC: hemoglobin 14.5 gm/dL, platelet count 299,000 cells/mcL, WBC 41,000 cells/mcL, vacuolated polymorphonuclear leukocytes were noted
- Electrolytes: Na+ 135 mmol/L, K+ 4.9 mmol/L, Cl- 95 mmol/L, HCO3- 18 mmol/L
- Renal function: creatinine 3.9 mg/dL, blood urea nitrogen (BUN) 59 mg/dL
- Liver enzymes: AST 294 (normal 8-48 U/L), ALT 303 (normal 7-55 U/L), ALP 187 (normal 45-115 U/L).
- Glucose: 58
Which of the following should be done immediately? (Click on the correct answer to proceed to the second of five pages)
Cite as: Raschke RA. April 2017 critical care case of the month. Southwest J Pulm Crit Care. 2017;14(4):134-40. doi: https://doi.org/10.13175/swjpcc039-17 PDF

Reader Comments