Morgan Wong, DO
Nicholas Villalobos, MD
Department of Internal Medicine
University of New Mexico
Albuquerque, NM USA
History of Present Illness
A 68-year-old man presented to the emergency department with a one-day history of lower back pain, arthralgias, and malaise. The patient had a previous splenectomy and was concerned about influenza.
Past Medical History, Social History, and Family History
He has a history of osteoarthritis, seasonal allergies, and splenectomy. He is a nonsmoker. Family history is noncontributory.
Physical Examination
Upon admission, the patient’s vital signs were notable for a temperature of 35.3 degrees Celsius, blood pressure of 74/44 mmHg, oxygen saturation of 85% on room air with a respiratory rate of 24 breaths per minute. Physical exam was prominent for non-pitting edema of the distal upper and lower extremities, as well as diffuse macular rash of the palms and soles.
Laboratory
CBC
- White blood cell count of 6.77 X103 cells/uL
- Hemoglobin of 13.8 gm/dL
- Hematocrit of 43.7%
- Platelet count of 19 x 103 /uL
Chemistry
- Creatinine of 3.0 mg/dL
- CO2 < 10 mmol/L
- Anion gap >18 mmol/L
- Liver function tests
- Alanine aminotransferase (ALT) of 511 U/L
- Aspartate aminotransferase (AST) of 529 U/L
- Total bilirubin of 1.0 mg/dL
Coagulation
- INR of 2.07
- Prothromin time of 22.5 seconds
- Partial thromoboplastin time of 82.3 seconds
- Fibrinogen level was 71 mg/dL
Arterial blood gases
- pH of 6.91
- pCO2 54 mmHg
- pO2 263
- HCO3 of 7.7 mmol/L
Procalcitonin >200 ng/ml.
His blood peripheral smear was examined.
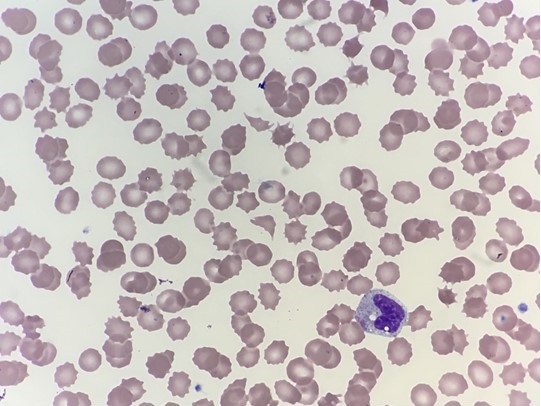
Figure 1: Peripheral blood smear on admission.
Given the results of the preliminary laboratory results and peripheral smear what hematologic abnormality are you most concerned with at this time? (Click on the correct answer to proceed to the second of five pages)
- Autoimmune hemolytic anemia (AIHA)
- Disseminated intravascular coagulopathy (DIC)
- Microangiopathic hemolytic anemia (MAHA)
- Thrombotic thrombocytopenic purpura (TTP)
Cite as: Wong M, Villalobos N. February 2017 critical care case of the month. Southwest J Pulm Crit Care. 2017;14(2):54-9. doi: https://doi.org/10.13175/swjpcc144-16 PDF